Schedule
Book a telehealth appointment from wherever you are. No insurance necessary.
Achieve your weight-loss goals with GLP-1 treatments like Wegovy® and Zepbound®, guided by licensed providers every step of the way.
Personalized care for women, with HRT and lifestyle support to ease menopause symptoms and restore balance.
Simple, supportive mental health care on your terms, including access to prescription medication when appropriate.
Connect with board-certified cardiologists to help manage blood pressure, cholesterol, and long-term cardiovascular risk — from the comfort of home.
Care without the wait—connect 24/7 with licensed providers for same-day prescription refills and common concerns like colds, flu, rashes, and more.
Talk to a doctor anytime, anywhere — 24/7 urgent & primary care with a telehealth visit in under one hour.
Get your medication prescribed online and sent same-day to your local pharmacy for pickup.
Save time, money, and the hassle — no in-person visits or insurance required.


Prescription treatments are tailored to your specific condition, ensuring effective relief.

Urgent evaluation is crucial to identify your condition early and prevent complications.
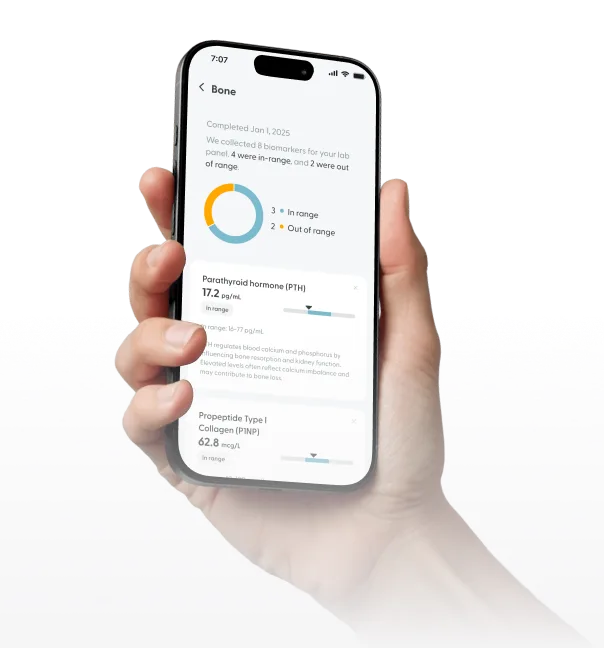
Accurate testing, if needed, can confirm your diagnosis and guide the best course of treatment

Licensed providers can send prescriptions to your local pharmacy within an hour, day or night.
step 1
Book a telehealth appointment from wherever you are. No insurance necessary.

step 2
Meet with a board-certified doctor or nurse practitioner from your mobile device.

step 3
Get a prescription if needed (save up to 90%), and pick it up at your pharmacy.
Irritable Bowel Syndrome (IBS) is a common chronic disorder that affects the large intestine (colon). It can cause a range of digestive symptoms, including abdominal pain, bloating, gas, diarrhea, and constipation.
IBS is typically managed through lifestyle changes, dietary modifications, and medication to help control symptoms and avoid flare-ups.
Get Started Get Started
Total Cholesterol

37 mg/mL
In range

LDL (Low-Density Lipoprotein)

47 mg/mL
In range

Triglycerides

158 mg/mL
Above range

A bile acid-binding resin that absorbs cholesterol-containing bile acids, which leave the body through stool. It may also be used to help stop IBS-associated diarrhea.
An anticholinergic that helps reduce the symptoms of stomach and intestinal cramping by slowing the natural movements of the gut and relaxing the muscles in the stomach and intestines.
A tricyclic antidepressant that helps with the symptoms of IBS, particularly when abdominal pain and diarrhea are the predominant symptoms. It can also be effective for bloating and nausea.
“Dr. Puopolo is a very knowledgeable doctor with vast experience in different medical fields. I feel I am in good hands.”
Verified Patient

“Great experience!! Never have done online telehealth before but for sure will again :)”
Verified Patient

“Dr. Culpepper was amazing. He explained things to me that I didn’t understand.”
Verified Patient

“Dr. Sehgal was amazing! Super helpful. She was answering my questions before I even asked. Very happy I picked her.”
Verified Patient

"The appointment went great. It was quick and easy, and the doctor was right on top of things!"
Verified Patient

Reviews shown are from verified LifeMD patients across various services. Photos are for illustrative purposes only.
While the exact cause of IBS is not fully understood, it is thought to be related to a combination of factors, including abnormalities in the nervous system, muscle contractions in the intestine, and changes in the gut microbiome.
The length and severity of IBS flare-ups can vary greatly depending on the person and the specific triggers involved. Some people experience mild symptoms that last only a few hours, while others may deal with more severe symptoms that can last for days or even weeks. IBS flare-ups can be triggered by stress, certain foods, hormonal changes, and other factors. Therefore, it’s important to know your triggers so you can take steps to avoid them.
No, IBS cannot be cured but it can be managed through lifestyle changes, medications, and stress management techniques. The treatment of IBS aims to alleviate symptoms such as abdominal pain, bloating, constipation, and diarrhea — and improve overall quality of life.
While the exact cause of IBS is unknown, certain foods can trigger symptoms such as abdominal pain, bloating, diarrhea, and constipation. Some of the worst foods and/or drinks for IBS include high-fat foods such as fried foods, processed foods, and fatty meats; dairy products such as milk, cheese, and ice cream; caffeine and alcohol; spicy foods; and artificial sweeteners. They can irritate the digestive system and exacerbate symptoms.
If you’ve been diagnosed with IBS, you can work with a healthcare provider or registered dietitian to develop a personalized diet plan that works for your individual needs.
While abdominal pain is a common symptom of IBS, it's also possible for the pain to radiate to other areas of the body, including the back. This is because the nerves that control the intestines also supply sensation to other areas of the body, including the back.
In addition, the muscle contractions that occur in the intestines during an IBS flare-up can also cause tension in the muscles of the back, leading to pain and discomfort. If you’re experiencing back pain, be sure to reach out to a healthcare provider so you can rule out any serious conditions.
No, IBS is not considered an autoimmune disease. Autoimmune diseases are conditions in which the body's immune system attacks healthy cells and tissues. IBS is a functional disorder of the digestive system that is characterized by a group of symptoms, including abdominal pain, bloating, constipation, and diarrhea.
While the exact cause of IBS is not fully understood, it’s thought to be related to a combination of factors, including abnormal muscle contractions in the intestines, changes in the gut microbiome, and abnormal communication between the brain and the gut.
While IBS can be uncomfortable and inconvenient at times, it’s not considered a dangerous or life-threatening condition — and it doesn’t cause physical damage to the digestive tract. However, IBS can impact a person's quality of life and can lead to anxiety, depression, and social isolation in extreme cases.
If you're living with IBS, a healthcare provider or registered dietician can help you take the right steps to avoid flare-ups.
Studies have shown that people with a family history of IBS are more likely to develop the condition themselves, suggesting that there may be a genetic predisposition to the condition. However, environmental and lifestyle factors also play a significant role.
If you have a family history of IBS, it’s a good idea to speak with a healthcare provider about strategies for reducing your risk of developing the condition, as well as ways to manage your symptoms if you’ve already been diagnosed.

Family Medicine
4.93 stars 170 reviews


Internal Medicine
4.98 stars 178 reviews


Internal Medicine
4.92 stars 261 reviews


Family Medicine
4.94 stars 178 reviews


Hormone Specialist
4.92 stars 163 reviews
