Schedule
Book a telehealth appointment from wherever you are. No insurance necessary.
Achieve your weight-loss goals with GLP-1 treatments like Wegovy® and Zepbound®, guided by licensed providers every step of the way.
Personalized care for women, with HRT and lifestyle support to ease menopause symptoms and restore balance.
Simple, supportive mental health care on your terms, including access to prescription medication when appropriate.
Connect with board-certified cardiologists to help manage blood pressure, cholesterol, and long-term cardiovascular risk — from the comfort of home.
Care without the wait—connect 24/7 with licensed providers for same-day prescription refills and common concerns like colds, flu, rashes, and more.
Talk to a doctor anytime, anywhere — 24/7 urgent & primary care with a telehealth visit in under one hour.
Get your medication prescribed online and sent same-day to your local pharmacy for pickup.
Save time, money, and the hassle — no in-person visits or insurance required.


Prescription treatments are tailored to your specific condition, ensuring effective relief.

Urgent evaluation is crucial to identify your condition early and prevent complications.
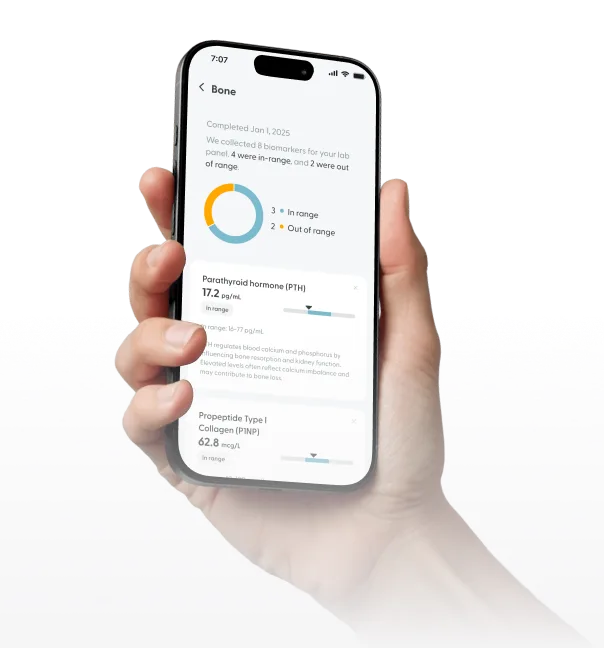
Accurate testing, if needed, can confirm your diagnosis and guide the best course of treatment

Licensed providers can send prescriptions to your local pharmacy within an hour, day or night.
step 1
Book a telehealth appointment from wherever you are. No insurance necessary.

step 2
Meet with a board-certified doctor or nurse practitioner from your mobile device.

step 3
Get a prescription if needed (save up to 90%), and pick it up at your pharmacy.
Lupus, or systemic lupus erythematosus (SLE), is a chronic autoimmune disease that occurs when the immune system mistakenly attacks the body's own tissues and organs, causing widespread inflammation and damage. Many people confuse lupus with other autoimmune conditions like rheumatoid arthritis or fibromyalgia. Lupus is a systemic autoimmune disease that can affect multiple organs including the skin, joints, kidneys, heart, and brain, whereas rheumatoid arthritis primarily targets the joints, and fibromyalgia causes widespread pain without actual organ inflammation or damage.
Lupus can cause a wide range of symptoms such as extreme fatigue, joint pain and swelling, a characteristic butterfly-shaped rash across the cheeks and nose, fever, hair loss, sensitivity to sunlight, and in severe cases, kidney problems or chest pain.
Getting the right treatment plan for lupus can help control symptoms, prevent flare-ups, protect organs from damage, and improve your quality of life while managing this chronic condition. With LifeMD, you can get immediate help and treatment guidance online without an in-office appointment. Prescription medications can effectively manage lupus symptoms and help prevent serious complications when used as part of a comprehensive treatment plan.
Get Started Get Started
Total Cholesterol

37 mg/mL
In range

LDL (Low-Density Lipoprotein)

47 mg/mL
In range

Triglycerides

158 mg/mL
Above range

Hydroxychloroquine is an antimalarial medication that works by modulating the immune system to reduce inflammation and prevent lupus flares. It's considered a cornerstone of lupus treatment and helps control symptoms like joint pain, skin rashes, and fatigue while reducing the risk of organ damage over time. It's typically taken once or twice daily long-term and is well-tolerated by most people. One of its major benefits is that it can help prevent lupus flares and reduce the need for higher doses of corticosteroids.
Prednisone is a corticosteroid that works by suppressing the immune system and reducing inflammation throughout the body. It's highly effective for controlling moderate to severe lupus symptoms and organ involvement, providing rapid relief during flares. It's typically taken once daily, with dosing adjusted based on disease activity. While effective, long-term use requires careful monitoring due to potential side effects like weight gain, bone loss, and increased infection risk.
Methotrexate is an immunosuppressant medication that works by reducing immune system activity and inflammation, helping to control lupus symptoms, particularly joint pain and skin manifestations. It's often used when hydroxychloroquine alone isn't sufficient or to allow for lower corticosteroid doses. It's typically taken once weekly as a pill or injection, along with folic acid supplementation to reduce side effects. Regular blood tests are required to monitor liver function and blood counts, but it can be highly effective for managing lupus with appropriate monitoring.
“Dr. Puopolo is a very knowledgeable doctor with vast experience in different medical fields. I feel I am in good hands.”
Verified Patient

“Great experience!! Never have done online telehealth before but for sure will again :)”
Verified Patient

“Dr. Culpepper was amazing. He explained things to me that I didn’t understand.”
Verified Patient

“Dr. Sehgal was amazing! Super helpful. She was answering my questions before I even asked. Very happy I picked her.”
Verified Patient

"The appointment went great. It was quick and easy, and the doctor was right on top of things!"
Verified Patient

Reviews shown are from verified LifeMD patients across various services. Photos are for illustrative purposes only.
Lupus has a genetic component, but it's not directly inherited in a simple way. If you have a family member with lupus, your risk of developing it is higher than the general population, but most people with lupus don't have a family history of the disease. Research shows that certain genes can increase susceptibility to lupus, but genetics alone don't cause it – environmental factors, hormones, infections, and other triggers also play significant roles. If one identical twin has lupus, the other twin has about a 25-30% chance of developing it, which shows that while genetics matter, they're not the only factor. Lupus is more common in certain ethnic groups, including African American, Hispanic, Asian, and Native American populations, suggesting a genetic predisposition in these communities.
The exact cause of lupus isn't fully understood, but it's believed to result from a combination of genetic, environmental, and hormonal factors. People with certain genetic variations are more susceptible, but environmental triggers like sunlight exposure, infections (particularly Epstein-Barr virus), certain medications, stress, or hormonal changes can activate the disease in those predisposed.
Lupus is much more common in women, especially during childbearing years, suggesting that hormones like estrogen play a role in triggering or worsening the condition. The disease occurs when the immune system becomes overactive and starts producing antibodies that attack the body's own tissues, causing widespread inflammation. Why this happens isn't completely clear, but it's likely a complex interaction between multiple factors rather than a single cause.
No, lupus is not currently curable. It's a chronic autoimmune condition that requires lifelong management. However, with proper treatment, many people with lupus can control their symptoms, prevent flares, protect their organs from damage, and live full, active lives. Treatment focuses on suppressing the overactive immune response, managing inflammation, and preventing complications.
Some people experience periods of remission where symptoms are minimal or absent, while others have more active disease requiring ongoing medication adjustments. Advances in treatment have significantly improved outcomes over the past few decades, and ongoing research continues to explore better therapies and potentially, one day, a cure.
Online lupus treatments typically involve a virtual consultation with a licensed healthcare provider. During the consultation, you can discuss your symptoms, describe which organs or systems are affected, provide your medical history including previous diagnoses and test results, and explain your current treatment regimen if you're already being managed for lupus. Your provider will assess your disease activity and determine if medication adjustments are needed or if new prescriptions are appropriate.
You'll then receive a personalized treatment plan with medication recommendations and any necessary prescriptions. Your healthcare provider may also recommend lifestyle modifications, sun protection strategies, and guidance on managing flares. However, lupus often requires specialist care from a rheumatologist and regular monitoring with blood tests and imaging, which may necessitate in-person visits.
It's important to be open and honest during your consultation to help your healthcare provider assess your lupus activity and treatment needs. Be sure to provide your doctor with detailed information, such as:
• Your symptoms, including which parts of your body are affected and how severe they are
• When you were diagnosed with lupus and what organs have been involved
• Current medications you're taking and how well they're controlling your symptoms
• Recent lab results or test findings if available
• New symptoms, worsening of existing symptoms, or signs of a flare
• Underlying health conditions, other medications, or any allergies
The more information you can provide, the better your doctor can assess your disease activity, adjust your treatment plan appropriately, and determine if you need additional testing or specialist referral.
LifeMD offers online lupus treatment guidance and can provide you with the prescriptions you need for symptom management and disease control. You can have these sent to your local pharmacy, where your medication will be prepared for pick-up. However, lupus management often requires coordination with a rheumatologist and regular monitoring, so online care works best as a supplement to ongoing specialist care or for medication refills and minor adjustments.
When it comes to treating lupus, the timeline varies significantly depending on the medication and severity of symptoms. Corticosteroids like prednisone often provide relief within days, reducing inflammation and controlling acute flares quickly. Hydroxychloroquine, a cornerstone lupus medication, takes much longer – typically one to three months before you notice significant improvement in symptoms like joint pain, rashes, and fatigue, with maximum benefits seen at six months or longer.
Immunosuppressants like methotrexate may take several weeks to months to show full effectiveness. Managing lupus is often a gradual process requiring patience and medication adjustments. The goal is long-term disease control and preventing organ damage rather than immediate symptom relief. If you don't see improvement after several weeks or if symptoms worsen, contact your healthcare provider for treatment adjustments or further evaluation.

Family Medicine
4.93 stars 170 reviews


Internal Medicine
4.98 stars 178 reviews


Internal Medicine
4.92 stars 261 reviews


Family Medicine
4.94 stars 178 reviews


Hormone Specialist
4.92 stars 163 reviews
